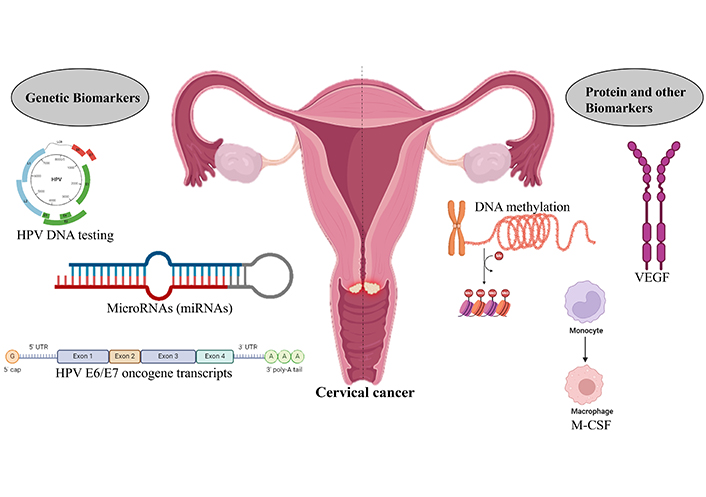
Human papillomavirus (HPV) is the major factor for cervical cancer. There are many strains of HPV, and it is indicated that more than 30 can infect the genital tract. Cervical cancer can be preventable through vaccinations, and the prognosis of cervical cancer can be better if detected early. Early detection through cervical tests or cytological screening can prevent cervical cancer progression. The most common cytology test or cervical test is a pap smear test. The pap results play an important role in the identification of precancerous lesions that allow your healthcare provider to develop a better treatment plan.
What is HPV?
Human papillomavirus has around 200 types. Some of them spread through vaginal, anal or oral sexual contact. These sexually transmitted HPV fall into the category of high-risk and low-risk. Low-risk HPV is harmless, while high-risk can lead to cancer. Regular pap results analysis is essential, especially for individuals who belong to high-risk groups.
What are high-risk HPV strains?
Among several HPV strains, twelve of them are considered high-risk HPV strains, including strains 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58 and 59. Among these, HPV 16 and 18 are responsible for the majority of HPV-induced cancers.
High-risk individuals for HPV
The individuals are considered to be at high risk for cervical cancer if they fall into any of the below categories:
- Individuals who have multiple sexual partners
- Individuals with HIV
- Immunocompromised individuals are more likely to get infected with HPV
- Smokers
- Individuals with other sexually transmitted diseases.
- Individuals engaging in early-age sexual activity pose a high risk of contracting sexually transmitted infections due to a lack of awareness
- Abnormal pap smear results often indicate the presence of HPV, which is a major risk of cervical cancer
How does the HPV can lead to cervical cancer?
HPV infects cervical cells and causes gradual changes in their structure. In most cases, the body’s immune system successfully eliminates HPV within one or two years, preventing long-term health issues. If high-risk HPV infection remains in the body, it can cause cellular changes leading to precancerous lesions. If left untreated, these lesions may develop into cervical cancer. The risk of cervical cancer increases by age after 30, making routine cervical screening essential.
The importance of cervical screening
Women with early-stage cervical usually do not experience symptoms. Symptoms typically appear when cancer has invaded the nearby tissue. Detecting abnormal cellular cervical changes early is crucial for preventing cancer from reaching an advanced stage. Three screening methods are used to detect cervical cancer.
Pap test
The pap test, also called pap smear test, screens for variations in cervical cells that might indicate precancerous or cancerous. It can also be done along with an HPV test.
Procedure: The procedure involves speculum insertion in the vagina to open it and view the cervix. A sample of mucus is collected from the cervix. The collected samples are subject to laboratory analysis.
Precautions before pap smear test
Avoid using tampons, birth-control foams, vaginal creams, lubricants or medicines for 7 days before the test. Do not douche for 2–3 days before the test. Avoid vaginal sex for 2 days before the test. These steps help ensure the most accurate results from your pap test.
The normal pap test result indicates no abnormal cells detected. The presence of typical cells indicates some minor changes but does not indicate cancer. If the pap smear test results show abnormal, it indicates further testing to determine the risk of cervical cancer.
HPV test
HPV test screens for the presence of human papillomavirus (HPV), which can cause genital warts and changes in cervical cells. This test identifies high-risk types of HPV that increase the risk of cervical cancer, helping guide further medical decisions.
When is an HPV test suggested?
- If your pap test results are atypical squamous cells of undetermined significance (ASCUS) and determined to be unclear
- Age 30 or older: Routine screening for women aged 30 and above
- Atypical screening history: If you have had abnormal cervical cancer screening results in the past
- For those who had a hysterectomy due to cervical cancer or abnormal cervical cells, the HPV test may be used to test vaginal cells
- HPV screening may start at age 35 for transgender women and men who have sex with men and at age 45 for others with HIV
- Individuals with severely atypical vulvar cells or vulvar cancer may start anal cell HPV screening within a year of diagnosis
Understanding the results
Positive HPV test: Indicates the presence of high-risk HPV but does not mean you will definitely get cervical cancer. It may lead to more frequent or extended screening
Negative HPV test: This indicates no signs of high-risk HPV and needs to be tested after 5 years
Pap/HPV co-test
Pap/HPV co-test indicates the testing of a pap test along with an HPV test simultaneously to screen for cervical cancer. HPV test detects DNA and RNA from high-risk types of HPV in cervical cell samples. Pap test results identify cervical cancer cells and precancerous changes in cervical cells. The same sample is usually used to process both tests. Women aged 30–65 are recommended to have Pp-HPV co-testing for every five years. This combined approach increases the accuracy of cervical cancer screening.
Preventive strategies
Reducing the risk of cervical cancer involves the following proactive steps:
- HPV vaccination, which protects against high-risk HPV strains
- Regular cervical tests and cytology tests, which can identify early changes
- Using protection to reduce HPV transmission
- Strengthening the immune system by adopting healthy lifestyle choices, supporting HPV resistance
Conclusion
HPV is a major contributor to cervical cancer, emphasising the need for awareness and prevention. Regular screenings and understanding pap results, as well as recognising the risk of survival cancer by age, are critical in early detection and treatment. Fortis, one of the best cancer hospitals in India, plays a key role in providing advanced care for cervical cancer and other types, ensuring that patients receive world-class treatment and support.